Paramedics walk gurneys back to a multi-patient transport bus at Kingston General Hospital on April 30 after dropping off COVID-19 patients from the Toronto area.
THE CANADIAN PRESS/Lars Hagberg
by Stephen L Archer, Professor, Head of Department of Medicine, Queen’s University, Ontario
You can learn a lot from a crisis. During Ontario’s COVID-19 pandemic, over 2,500 patients have required transfer from Toronto to receive life-saving care in other cities.
The egress of COVID-19 patients from Toronto began in mid-November 2020, when the Ontario government activated the GTA Hospital Incident Management System. Transfers peaked in April during the third wave of COVID-19.
At Kingston Health Sciences Centre (KHSC) we have received over 100 Toronto area patients with COVID-19, many on ventilators. They came by helicopter, ambulance and even by bus, unaccompanied by family.
Ontario even put out a national call for health-care workers to help out, and Newfoundland answered.
Why would Ontario need to transfer masses of critically ill patients with a highly infectious disease across the province, even resorting to involuntary transfers? Why would a metropolis like Toronto call on comparatively tiny Newfoundland for health-care workers? Is this simply the unavoidable consequences of a huge third wave of COVID-19?
In fact the root causes began long before the pandemic and originated with a flawed understanding of the capacity (physical and human) of our health-care system.
Two fallacies
I lead the department of medicine at Queen’s University and co-lead the medicine program at KHSC. In these roles I am responsible for hiring doctors and ensuring our medicine beds run efficiently. I have often been confronted by two fallacies relevant to the genesis of our current crisis:
- Fallacy 1 — Ontario has enough hospital beds because medical care is largely conducted on an outpatient basis.
- Fallacy 2 — Canada has more than enough health-care workers and doctors.
Both fallacies have been widely embraced by provincial and federal governments. Let’s examine the validity of these beliefs with the goal of designing a more resilient health-care system.
Fallacy 1: Number of hospital beds

THE CANADIAN PRESS/Paul Daly
It is popular in Canada to believe that the future of medicine is mostly in outpatient care and that hospital beds are obsolete. In reality, as medicine becomes more high-tech, admissions are shorter but more beds are needed to support procedures that improve the quality and duration of life.
We are now putting heart valves, hips, lenses and more into older Canadians, and performing lifesaving diagnostic and therapeutic interventions on people who 20 years ago would have been considered ineligible because they were too premature, too obese or too high-risk.
Canada’s bed shortage is particularly critical in academic health sciences centres that uniquely deliver advanced forms of care. Pre-pandemic Ontario was running at 96 per cent occupancy.
Our bed capacity was designed for troughs in demand, like summer, not for peaks, as occur each fall when influenza strikes. Every fall, as rates of infections like influenza rise, our emergency departments and medicine wards become congested and admitted patients must be accommodated in hallways. These are the consequences of inadequate numbers of in-patient beds. The COVID-19 pandemic simply made our tenuous reserve capacity more apparent.
Ontario has built new bed capacity for COVID-19, but had minimal reserve capacity pre-pandemic.
Ontario Health did three things to deal with COVID-19:
- Relocated 1,000 people from hospitals, including alternative level of care patients;
- Cancelled “elective procedures” and repurposed the resulting 6,849 beds for possible COVID-19 patients (necessary but dangerous to the health of the 99 per cent of Canadians that don’t have COVID-19; and
- Opened 2,500 new hospital beds.
The government views Ontario’s health-care system as “one resource.” That sounds good in principle, but moving patients on ventilators away from their families is a poor way to deliver care. In addition, most of Ontario’s COVID-19 capacity derives from deferring elective procedures, few of which are truly elective.
The simple truth is we were never configured to deal with surges in admissions. We mistakenly focused on the symptoms of bed deficiency, like “hallway medicine” and emergency room wait times and failed to address the root cause: inadequate numbers of beds (in hospitals and long-term care facilities).

THE CANADIAN PRESS/Nathan Denette
Several caveats about this bed-centric article are relevant. First, outpatient care is important and when it fails, unnecessary hospitalizations occur.
Second, inadequate long-term care facilities and home care services in the community exacerbate the bed shortage by causing inappropriate hospitalization of people awaiting alternate levels of care.
Third, don’t let the term “hospital bed shortage” mislead you to envision a shortage of mattresses and pillows; a “bed” is a surrogate for the capital and human resources required to provide care in that bed 24/7, 365 days a year.
Fallacy 2: Number of health-care workers
Canada has 86,092 active physicians (excluding trainees), 25 per cent of whom are international medical graduates. When recruiting academic physicians, I often struggle to find a Canadian-trained doctor and rely on our pool of international medical graduates. These doctors are often first-rate, but the fact we rely on other countries to train our doctors is not widely recognized.
Our dependence on international medical graduates does not reflect Canadians not wanting to become doctors. Queen’s University School of Medicine has 5,000 applicants for 100 seats and more Canadians are training abroad as physicians than in Canada. The Organization for Economic Co-operation and Development (OECD) tracks medical graduates per 100,000 inhabitants in member countries. Canada is near the bottom.
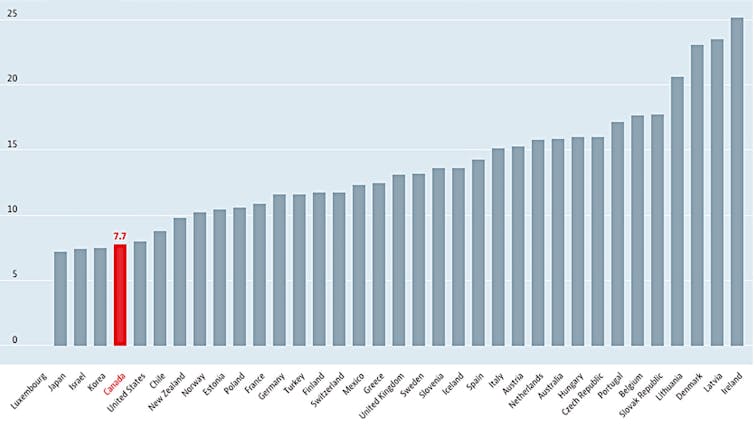
(OECD data)
Our physician-to-population ratio is also low, ranking 29 out of 36 OECD nations. The reality is that doctors and other health-care workers are expensive. Canada’s universal health-care system has many advantages; however, a single-payer system means the provincial governments (the payers) see a whopping human resources bill every year and, in trying to control costs, are invested in keeping numbers of physicians (and hospital beds) in check.
COVID-19 has given us a master class in what is wrong with our health-care system. Admittedly, Canada’s post-pandemic to-do list is long and includes improving the care of seniors, providing affordable child care, fostering a domestic biotech industry, re-establishing a pandemic surveillance system and bolstering public health programs. We also need to legislate good employment practices, such as provision of paid sick days.
Additionally, we need to continue the funding for the new beds created to deal with the pandemic, using them flexibly to ensure we have surge capacity. We should also create an adequate supply of domestically trained health-care professionals.
It is clear what must be done. We must find the funds and will power to meet the post pandemic moment with action.
04/26/2024 Source of data Below: Civil Society Solidarity Partners against COVID-19
Population: 41,014,164 adjusted for estimated real COVID-19 deaths
| Canada | Cases | Deaths | Cured | Active |
| Reported: | 4,949,441 | 59,139 1.2% CFR | 4,878,112 | 12,190 |
| Estimate: | 27,370,409 | 76,880 *0.28% IFR | 26,975,959 | 67,411 |
*Inferred IFR is an estimate only. The actual COVID-19 IFR may not be accurately calculated for the entire human race until long after the pandemic has ended.
Below: Extensive Estimates using data from multiple sources.
Beta experimental estimates for Canada. Reported + unreported mild + asymptomatic COVID-19 infections.
The total actual number of infections in Canada including all the untested, unreported, asymptomatic infections is likely greater than 27,370,409 (66.73% of the population) including mild and asymptomatic cases. That would mean the estimated inferred average Infection Fatality Rate: (IFR) is likely around 0.28%
Canadian COVID-19 deaths to 2024-04-25 are estimated to be 76,637 Using estimated IFR of 0.28%. Global average 0.44% Global estimated inferred average Infection Fatality Rate (IFR
76,637 (0.28% IFR) is the CSPaC estimated number of Canadian COVID-19 deaths (based on the inferred IFR) including those deaths unreported as COVID-19). The IHME estimates excess deaths in Canada to reach much higher than CSPaC estimates.
See The Lancet estimate of excess mortality from COVID-19 (Download PDF) in 191 countries/territories and 252 subnational units of select countries, from 1 January 2 0 2 0, to 31 December 2 0 2 1.
76880 Is the CSPaC estimated number of Canadian COVID-19 deaths based on a modified universal algorithm which factors more sophisticated public health infrastructure and also fewer available urgent care beds and facilities which is a problem in much of Canada in an emergency measures context.
The closeness of the two numbers derived from unique data and methods suggests their high probability. The blended data of three projections from three different biostatistician labs also confirms the estimates +/- .01%.
It is safe to say that Canadians have endured the grief of losing 76880 family members. Every number has a face. May their memory be forever a blessing to their families and friends.
Canada's advanced public health standards.
Canada and the USA have Infection Fatality Rates close to global averages but since vaccine booster-rates have dropped, CFR in both countrioes is climbing slightly above global averages. (influenza has an IFR of .1% or 6 per 100k (2019)).
Ontario, Canada Reports no longer updated. See Archives to 5 March 2023
Below: CSPAD estimated 2024-04-25 22:05 GMT COVID-19 data for India.
EPICENTER-2: India (45,035,393)
| Reported | *Cases | *Deaths | *CFR | *Recovered |
| India | 45,035,393 | 533,570 | 1.2% | 0 |
Note: India's reported death sum and cured data are widely seen among epidemiologists and biostatisticians as unreliable. For example, 3,094,653 is CSPAD estimated sum of deaths while India reports 533,570, creating the largest discepency in the world. India might only report hospital tested cases. Sources among hundreds of nurses and other medical practitioners provide a picture that in summary concludes most cases never present in a hospital especially in northern provinces where health care is less available and utilization is low anyway because of poverty, hence most people die at home in India. This theory could explain discrepancies between reported data and algorithmic estimates.
| Locale | Cases | Deaths | Active |
| India reported: | 45,035,393 | 533,570 | 44,501,823 |
| India estimates: | 249,045,723 | 3,094,653 | 245,951,070 |
Data collected and reported by: Civil Society Solidarity Partners against Disease