(Shutterstock)
Chris Bauch, University of Waterloo; Brendon Phillips, University of Waterloo; Dillon Thomas Browne, University of Waterloo, and Madhur Anand, University of Guelph
Formulating school and childcare center reopening plans in North America this fall has been a daunting task, as both the pandemic and our scientific knowledge of COVID-19 continue to unfold quickly.
For students attending in person, there are many questions to consider: How important is the cleaning and disinfecting of surfaces? Which age of students should use masks, and when? What is the best approach to cohorting? How large should class sizes be?
Knowledge of how COVID-19 spreads has improved since the pandemic started, but as reopening plans were being developed, we recognized a need to investigate outbreak scenarios in schools and childcare centres. With our combined background in mathematical modelling, epidemiology, environmental sciences and childhood education, we tackled the question of class sizes.
We developed a mathematical model of outbreaks in homes and classrooms. The model made a very surprising prediction: as class sizes go up, the negative impacts of COVID-19 go up exponentially faster.
A granular approach
We opted for an “individual-based” model where distinct individuals (adults and children) are allowed to interact according to specified rules. This highly granular approach allows us to see the effects of social groupings and individual characteristics on personal outcomes like missed school days.
Using age and household size information obtained from Canadian census data, we constructed small populations with childhood education centres and associated households consisting of one or more adults and one or more children. Our model is essentially a simulated virtual world of schools and homes.
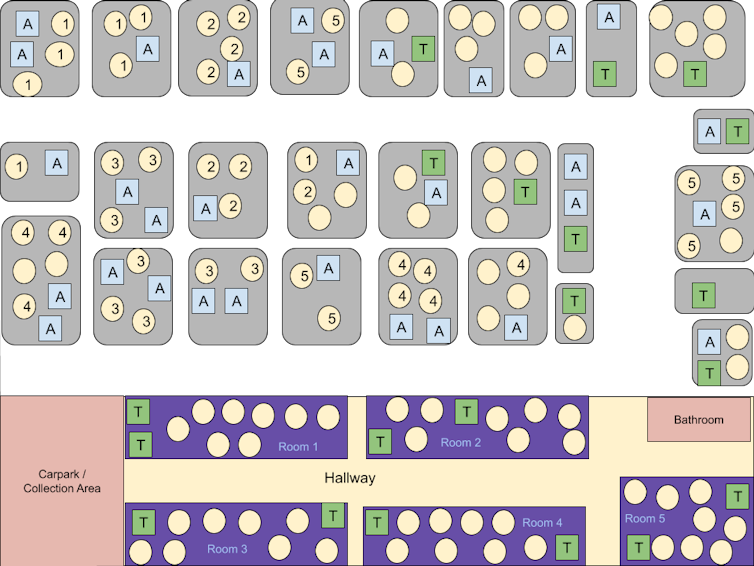
(Chris Bauch), Author provided
Children were allocated to classrooms randomly or by grouping siblings together. We considered childcare center scenarios with student/educator ratios of 7:3, 8:2 and 15:2. We also considered primary school scenarios with student/educator ratios of 8:1, 15:1 and 30:1. Students could attend class every day or alternate between in-person instruction one week and online learning the next week.
Influencing factors
Then we ran our computer simulation of COVID-19 outbreaks in this setting. We assumed that when a symptomatic case of COVID-19 appears in a classroom that it would then be closed for 14 days.
But modelling the impact of class sizes on outbreaks is tricky.
Schools have been closed during much of the first wave and so — perhaps unsurprisingly — school-aged children did not account for a significant portion of cases during this period. In addition, children are more likely to be asymptomatic and therefore not reported as having COVID-19. A host of other factors could influence both the risk and size of outbreaks.
So how can we predict what outbreaks in schools might look like, given that schools have not been open in Ontario since March 2020? Since we don’t know all of the right input values to use, we took an approach of “uncertainty analysis,” a cornerstone of scientific inquiry — admitting that you do not know everything.
This approach meant that we would change the model inputs and study how those affect the predictions. For example, we distinguished between a “high transmission” assumption, where the virus can spread quickly, and a “low transmission” assumption, where the virus spread is being slowed by the use of masks, disinfection and physical distancing.
Triple whammy
Across all of the permutations used in our uncertainty analysis, we were surprised to find that when class size doubled, the number of cases and student-days lost to closure more than doubled. Student-days are calculated by multiplying the number of closure days by the number of students affected, and with each class size doubling, they went up by factors of two to five.
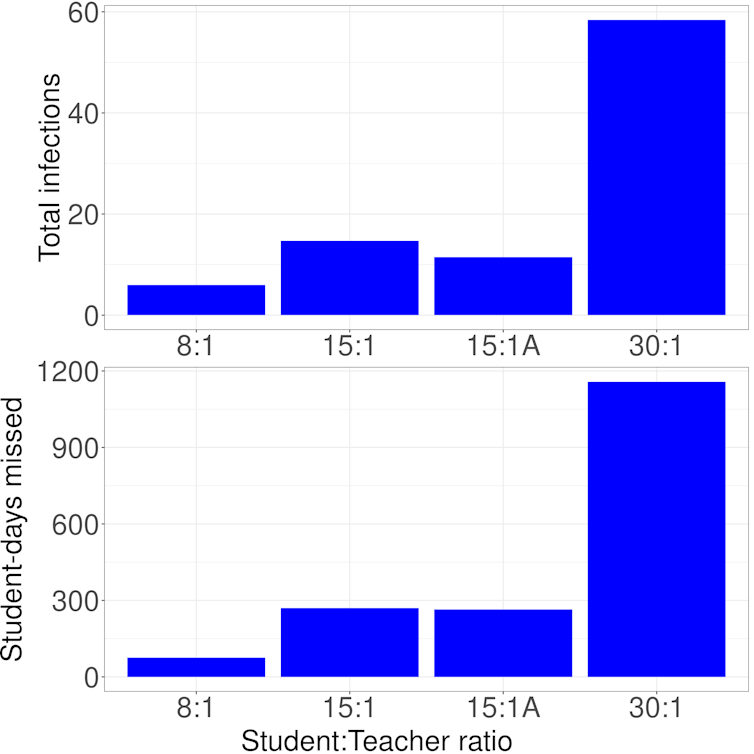
(Chris Bauch), Author provided
When we increased the transmission rate, it changed the total number of cases, but the relative number of cases or student-days lost to closure between the various class size scenarios did not change much: larger classes were always relatively worse than smaller classes, and by about the same factor of two to five.
We describe this as a “triple whammy.” First, when class sizes are larger, the chances are higher that one of the children will test positive. Second, when that child does test positive and the class is closed, closure of a larger class affects more children. Third, by the time the case is identified, the student might have been transmitting the virus for several days, or someone else in the class may have been asymptomatic and transmitting for many days. This third point is crucial — it is increasingly clear that SARS-CoV-2 can be spread by aerosol particles.
Other consequences
The worst scenario, by a wide margin, was the 30:1 ratio in the primary school setting. Switching to a 15:1 ratio with alternating weekly cohorts (15:1A) reduced the number of cases and student-days lost to closure by a factor of around four. And even though higher student/educator ratios allow more students to get in-person instruction, they also cause more disruptions due to more frequent need to close classrooms when a case is identified.
In addition, there are likely to be significant psychological, social and mental health consequences for parents and children when schools and childcare centres close. And since outbreaks can happen at any time, working parents may need to be pulled from their work with little or no advance notice.
Moving forward
Schools and childcare centers have already reopened. Some districts have been allowed to go with a preferred model that permits smaller class sizes, and this is a step in the right direction.
There are also many examples of how school districts can reduce class size at minimal cost. For instance, kindergarten classes with two teachers could split into two groups, one of which uses the library, gym or spends more time outdoors in activities.
If widespread school closure occurs again this fall, we suggest that re-reopening plans pay close attention to the aspect of class size. While the risk of outbreaks will never be zero even with small classes, it would be prudent for class sizes to be lower, so these disruptions affect the fewest number of children and families possible. In the meantime, for parents and caregivers, the best thing to do is have honest and open conversations around how closures will look like in their family, including arrangements for work and child care. The math tells us that school or classroom closures will be a reality for many school districts this fall.![]()
Chris Bauch, Professor of Applied Mathematics, University of Waterloo; Brendon Phillips, Ph.D. student, Applied Mathematics, University of Waterloo; Dillon Thomas Browne, Assistant Professor, Psychology, University of Waterloo, and Madhur Anand, Professor & Director, Global Ecological Change & Sustainability Laboratory, University of Guelph
This article is republished from The Conversation under a Creative Commons license. Read the original article.
04/19/2024 Latest Canadian COVID-19 Data
Population: 40,494,107 adjusted for estimated real COVID-19 deaths
| Canada | Cases | Deaths | Cured | Active |
| Reported: | 4,946,090 | 59,034 1.2% CFR | 4,881,312 | 5,744 |
| Estimate: | 27,351,878 | 76,744 *0.28% IFR | 26,993,655 | 31,764 |
*Inferred IFR is an estimate only. The actual COVID-19 IFR may not be accurately calculated for the entire human race until long after the pandemic has ended.
Below: Extensive Estimates using data from multiple sources.
Beta experimental estimates for Canada. Reported + unreported mild + asymptomatic COVID-19 infections.
The total actual number of infections in Canada including all the untested, unreported, asymptomatic infections is likely greater than 27,351,878 (67.55% of the population) including mild and asymptomatic cases. That would mean the estimated inferred average Infection Fatality Rate: (IFR) is likely around 0.28%
Canadian COVID-19 deaths to 2024-04-15 are estimated to be 76,585 Using estimated IFR of 0.28%. Global average 0.49% Global estimated inferred average Infection Fatality Rate (IFR
76,585 (0.28% IFR) is the CSPaC estimated number of Canadian COVID-19 deaths (based on the inferred IFR) including those deaths unreported as COVID-19). The IHME estimates excess deaths in Canada to reach much higher than CSPaC estimates.
See The Lancet estimate of excess mortality from COVID-19 (Download PDF) in 191 countries/territories and 252 subnational units of select countries, from 1 January 2 0 2 0, to 31 December 2 0 2 1.
76744 Is the CSPaC estimated number of Canadian COVID-19 deaths based on a modified universal algorithm which factors more sophisticated public health infrastructure and also fewer available urgent care beds and facilities which is a problem in much of Canada in an emergency measures context.
The closeness of the two numbers derived from unique data and methods suggests their high probability. The blended data of three projections from three different biostatistician labs also confirms the estimates +/- .01%.
It is safe to say that Canadians have endured the grief of losing 76744 family members. Every number has a face. May their memory be forever a blessing to their families and friends.
Canada's advanced public health standards.
Canada and the USA have Infection Fatality Rates close to global averages but since vaccine booster-rates have dropped, CFR in both countrioes is climbing slightly above global averages. (influenza has an IFR of .1% or 6 per 100k (2019)).